Lyme Disease Guidelines for 2023
Up to 50% of the black-legged ticks in the KFL&A region carry Borrelia, the bacteria associated with Lyme disease.1 Ticks also carry an incredible number of other infections – many of which we’re just starting to understand. Treat every tick bite with immune-supportive measures and know when to request antibiotics from your doctor. Review these updated 2023 guidelines and reach out if you’re uncertain or need additional support.
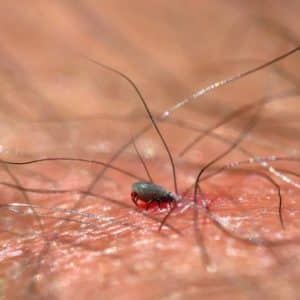 I’ve received a lot of calls lately from panicked patients with a tick bite and a rash at the bite site. Their question: Is this a Lyme Disease rash and do I need to go get antibiotics?
I’ve received a lot of calls lately from panicked patients with a tick bite and a rash at the bite site. Their question: Is this a Lyme Disease rash and do I need to go get antibiotics? 
 We’re pleased to introduce a versatile technology to our clients and patients that we believe aligns with the body’s ability to heal: a “Photobiomodulation” device by Inlight Therapy.
We’re pleased to introduce a versatile technology to our clients and patients that we believe aligns with the body’s ability to heal: a “Photobiomodulation” device by Inlight Therapy.  Many people still assume that electromagnetic fields (EMFs) emitted by their devices (cell phones, computers and ipads, etc.) are completely harmless. This conventional believe persists despite thousands of research studies that identify EMFs as an obstacle to the body’s natural repair mechanisms.
Many people still assume that electromagnetic fields (EMFs) emitted by their devices (cell phones, computers and ipads, etc.) are completely harmless. This conventional believe persists despite thousands of research studies that identify EMFs as an obstacle to the body’s natural repair mechanisms. What is Lyme Disease? This question seems simple enough, and perhaps for the people who successfully recover on their own or with an antibiotic, the answer is simple. But for the 5% to 20% of individuals who develop persistent, debilitating symptoms for months to years after the initial infection, the definition is anything but simple. Depending on the circle you run in, the illness is called Chronic Immune Dysfunction (CID), Multi-Systemic Infectious Disease Syndrome (MSIDS), Post-Treatment Lyme Disease Syndrome (PTLDS), Chronic Lyme Disease, Persistent Lyme Disease, or it plain just doesn’t exist.
What is Lyme Disease? This question seems simple enough, and perhaps for the people who successfully recover on their own or with an antibiotic, the answer is simple. But for the 5% to 20% of individuals who develop persistent, debilitating symptoms for months to years after the initial infection, the definition is anything but simple. Depending on the circle you run in, the illness is called Chronic Immune Dysfunction (CID), Multi-Systemic Infectious Disease Syndrome (MSIDS), Post-Treatment Lyme Disease Syndrome (PTLDS), Chronic Lyme Disease, Persistent Lyme Disease, or it plain just doesn’t exist.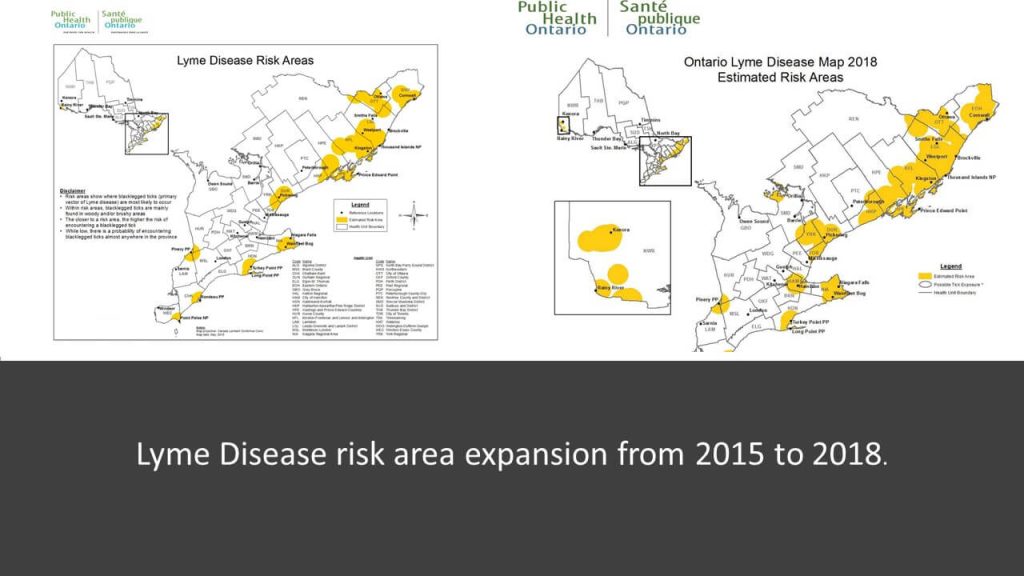
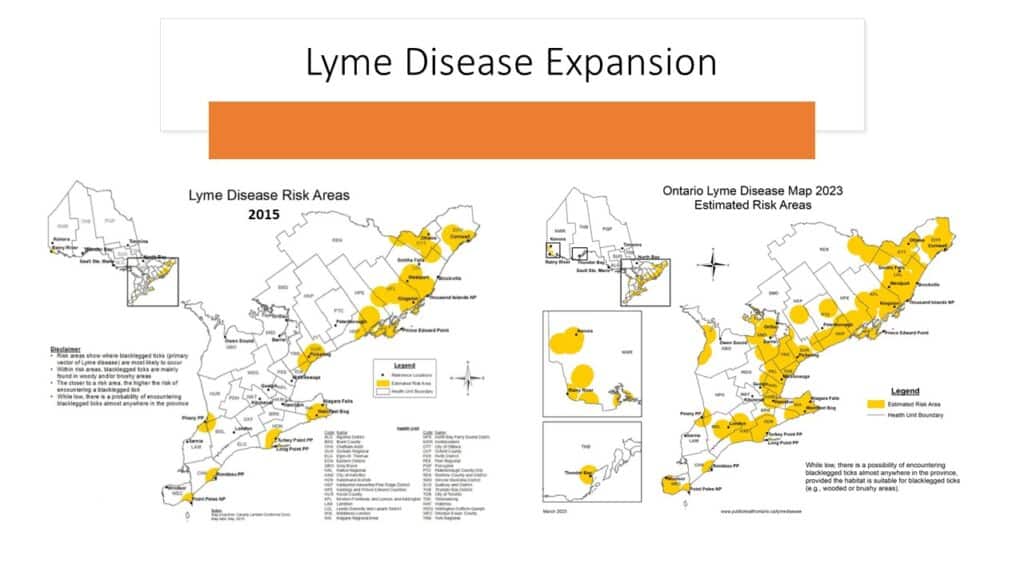
 Where did this Lyme epidemic come from? “Tick-checks” weren’t a thing when we were kids. Now, ticks not only swarm our conservation areas, but also our gardens and children’s playgrounds. More than 1/3 of them in our area are infected with Borrelia, the bacteria believed to cause Lyme Disease, and an unknown number are infected with Lyme “co-infections” such as Bartonella and Anaplasma. Our instinctual response to this threat is to kill tick populations as quickly as possible… But history, ecological principles, integrative medicine and current research all teach us that this approach doesn’t work. A more sophisticated approach, one that acknowledges underlying causes of this epidemic, is urgently required.
Where did this Lyme epidemic come from? “Tick-checks” weren’t a thing when we were kids. Now, ticks not only swarm our conservation areas, but also our gardens and children’s playgrounds. More than 1/3 of them in our area are infected with Borrelia, the bacteria believed to cause Lyme Disease, and an unknown number are infected with Lyme “co-infections” such as Bartonella and Anaplasma. Our instinctual response to this threat is to kill tick populations as quickly as possible… But history, ecological principles, integrative medicine and current research all teach us that this approach doesn’t work. A more sophisticated approach, one that acknowledges underlying causes of this epidemic, is urgently required. In medicine, when an infection becomes chronic, we generally consider that either the immune system is failing to control the infection, such as in HIV and AIDs, or that the infection is able to hide from the immune system, such as with the herpes virus that causes cold sores. Evidence suggests that chronic infection with any of the microbes associated with Lyme disease falls into both categories, which is one reason why persistent symptoms are so difficult to treat.
In medicine, when an infection becomes chronic, we generally consider that either the immune system is failing to control the infection, such as in HIV and AIDs, or that the infection is able to hide from the immune system, such as with the herpes virus that causes cold sores. Evidence suggests that chronic infection with any of the microbes associated with Lyme disease falls into both categories, which is one reason why persistent symptoms are so difficult to treat.  Chronic Lyme Disease (and the many labels we’ve come to use to describe persistent symptoms after a tick bite) is complex, involving physical, emotional, and spiritual aspects of health. Like the great Eastern gurus who guide their students to deeper levels of self-awareness, Lyme disease pushes people to more fully develop their faith and spirituality. A patient who has healed from chronic symptoms has done a lot of soul searching and practiced forgiveness and gratitude. This guru teaches us many lessons, including the paradigm-shifting awareness of what an “infection” is. Chronic Lyme Disease doesn’t classify.
Chronic Lyme Disease (and the many labels we’ve come to use to describe persistent symptoms after a tick bite) is complex, involving physical, emotional, and spiritual aspects of health. Like the great Eastern gurus who guide their students to deeper levels of self-awareness, Lyme disease pushes people to more fully develop their faith and spirituality. A patient who has healed from chronic symptoms has done a lot of soul searching and practiced forgiveness and gratitude. This guru teaches us many lessons, including the paradigm-shifting awareness of what an “infection” is. Chronic Lyme Disease doesn’t classify.